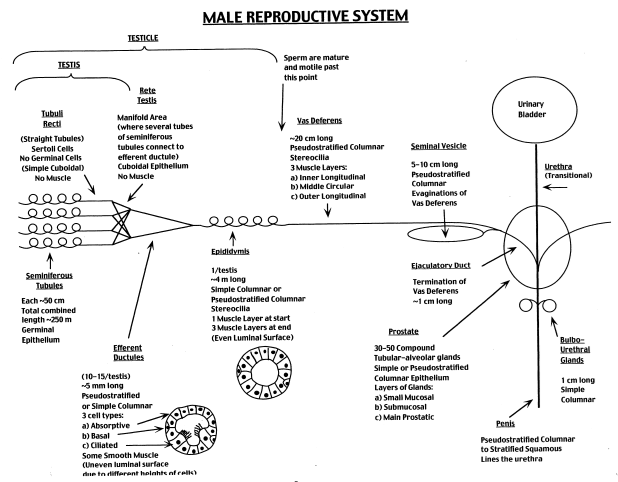
Male Reproductive System |
||
| Atlas (Wheater's 6th ed.): | ||
| Text (Junquiera's 15th ed.): | ||
Overview: The goal of this lab is to examine the histology of the principal parts of the male reproductive tract. Use Junquiera's or Wheater's texts and the diagram (below) as guides. Understand the functional correlates of the architecture you observe, and be able to distinguish each of the components. Pay attention to the disposition of the epithelium, note the special modifications of tubules and glands, and observe the amount and layering of connective tissue and smooth muscle.
Slide DescriptionsWebslide 0087_M: Testis, human, 19 yr. M, Masson [DigitalScope] Note the following on this thick section:
Webslide 0275_M (courtesy of U. of Mich.): Testis, human, H&E [DigitalScope] This section features part of the testis on the lower portion of the slide. Note the seminiferous tubules and Leydig cells. Present on the right hand side of the tunica albuginea is the mediastinum, a thickened portion of the tunica albuginea that contains the rete testis. The rete testis, the area where tubules coalesce and connect to efferent ductules, is shown as irregularly-shaped lumens lined by a simple cuboidal epithelium. Beyond the rete testis are efferent ductules with pseudostratified epithelium and prominent tufts of cilia. The upper right hand portion of the slide contains both efferent ductules and epididymis.
Webslide 0031_M: Testis, hamster, 1.5 µm, AF-TB [DigitalScope] Observe the following in this well-preserved thin section:
Webslide 0088_M: Epididymis, monkey, Orange G stain [DigitalScope] Note the following:
Webslide 0089A_M: Vas deferens, human, H&E [DigitalScope] Webslide 0089B_M: Vas deferens, human, 19 yr. M, H&E [DigitalScope] Although both slides are from the vas deferens, one is taken from the proximal duct while the other is taken from the distal portion near the seminal vesicles. Which slide is taken from which portion of the vas deferens? How can you tell? Note the following: 1. Three robust layers of smooth muscle at the start of the vas deferens.
Webslide 0090_M: Seminal vesicle, monkey, H&E [DigitalScope] Note the following:
Webslide 0054_M: Seminal vesicle, human, 19 yr., Mallory trichrome [DigitalScope] Use this slide to study the same aspects of the seminal vesicle as you did for Webslide 90. However, in this slide the smooth muscle is much more obvious due to the staining.
Webslide UMich 281: Prostate, human, H&E [DigitalScope] See also: Webslide 0091_M: Prostate, human, Orange G [DigitalScope] The prostate in an adult is about the size and shape of a chestnut and contains 15-30 tubuloalveolar glands that empty separately into the prostatic urethra. The most important structures to see on the slide are the prostatic glands that are present over most of the section. The glands are embedded in a fibromuscular stroma that includes abundant smooth muscle. The epithelium of the glands is simple or pseudostratified columnar (there may be a few basal cells), and the cells differ greatly in height to give the epithelium a folded appearance. The prostatic urethra can also be seen (it has a stratified epithelium several cells thick and numerous mucosal glands). Also present is the prostatic utricle flanked by paired ejaculatory ducts. With these landmarks, one can identify the various zones of the prostate that are clinically relevant in their propensity to become hyperplastic and/or cancerous:
Webslide UMich 282: Prostate, human, H&E [DigitalScope] Use this slide to examine the tubuloalveolar structure of the prostate glands, the smooth muscle between the glands, and at the concretions that are commonly seen within these glands.
Webslide UMich 286: Glans penis, human, H&E [DigitalScope] Note the following: 1. Urethra with both stratified squamous and transitional epithelium present.
PATHOLOGY CORRELATE CASE NUMBER 5 (slide courtesy of UIowa) Clinical History: A 77-year-old man went to his primary care physician for an annual checkup. Digital rectal exam revealed a firm nodule at the base of the prostate gland. Serum PSA was measured at 7.0 ng/mL (normal < 4.0 ng/mL). Needle biopsies were performed and histopathology showed the presence prostatic adenocarcinoma with a Gleason grade of 3+4. The patient subsequently underwent a total prostatectomy. (1) Features that confirm this is a prostate specimen:
(2) Features consistent with a diagnosis of prostatic adenocarcinoma:
(3) Feature consistent with the Gleason grade of 3+4=7:
I. TESTIS270 testis, human, H&E [Orientation] [DigitalScope] These slides (except for the UCSF slide and Duke Webslide) include both testis and epididymis (you will study epididymis later in this laboratory session): the testis is the larger of the two structures on the slide. The capsule of the testis is composed of dense connective tissue and is called the tunica albuginea. Within the testis you will see numerous profiles of seminiferous tubules, with interstitial tissue between them. In the interstitial tissue between the seminiferous tubules are clusters of Leydig cells, which secrete the male steroid hormone, testosterone. These are the most prominent cells in the interstitial tissue (best seen in #270 [example], or #275 [example]). Also visible in the interstitial tissue are blood vessels and smaller cells characteristic of loose connective tissue. Now take a closer look at the the seminiferous tubules in #270 [example] [Orientation] or #270 [example] [Orientation] (in some of the seminiferous tubules the epithelium may be pulled away somewhat from the basement membrane, leaving a white space, which is an artifact). Each seminiferous tubule is surrounded by a boundary layer or tunica propria, composed of flattened cells, several cells thick. Most of the cells that lie against the basement membrane and have round nuclei are spermatogonia. Don’t worry about distinguishing between type A and type B spermatogonia. Now look for considerably larger nuclei midway up in the epithelium that are also round and are filled with a tangle of dense chromosomes. These are the nuclei of relatively mature primary spermatocytes, which are in the extended prophase of the first meiotic division. These are numerous but unfortunately not always well preserved (the nuclei may be somewhat swollen or distorted). All of the smaller cells in the upper half of the epithelium (toward the lumen of the tubule) are spermatids in various stages of differentiation into mature sperm. The spermatids initially have round nuclei, but these gradually become smaller, denser and assume the shape of sperm heads. The smallest black structures you see are the heads of mature spermatids about to be released into the lumen. Their tails are difficult to make out. Now look for Sertoli cell nuclei, which are large, relatively pale and irregular in shape, and contain a prominent nucleolus (sometimes out of the plane of section). Their nuclei commonly occur just above (toward the lumen from) the spermatogonia. Secondary spermatocytes are rarely seen, since almost immediately after they arise they undergo the second meiotic division to become spermatids. If you are anxious to see secondary spermatocytes, find division figures and look around them for nuclei that are intermediate in size between those of primary spermatocytes and spermatids. They are hard to find, so don’t spend much time looking. How can you differentiate between Sertoli cells, spermatogonia and primary spermatocytes?
II. MEDIASTINUM and EPIDIDYMIS270 testis, human, H&E [Orientation] [DigitalScope] Returning to the slides of the seminiferous tubules, study the passageway by which the sperm pass from the seminiferous tubules through the rete testis, efferent ducts and epididymis to reach the tail of the epididymis, where they are stored in preparation for an ejaculation. Scan along the tunica albuginea of the testis, looking for a region where it thickens and is permeated by a network of flattened channels in the dense connective tissue. This portion of the testis is known as the mediastinum; the network of channels is the rete testis and is probably best seen in slide #270. Observe that the rete testis is lined with a cuboidal (or sometimes low-columnar) epithelium and you may see occasional microvilli. (Purely as an aside, these cells also have a single or “primary” cilium. Obviously, these cilia don’t contribute much in the way of helping to propel sperm through the channel. Instead, they may function as chemoreceptors allowing the lining cells to monitor and modify the luminal contents). The sperm leave the testis by means of these channels to reach the efferent ducts. However, for now, shift your attention outside the testis to the part of the epididymis that is included in this slide. You will see numerous sections through the long and convoluted duct that makes up the epididymis apparent in #270 [CAVEAT] . The epithelium of the duct is pseudostratified columnar. The tall epithelial cells have long microvilli on their apical surface (sometimes called “stereocilia”, although they are not cilia at all). You may be able to make out a thin layer of smooth muscle around the tubules, which presumably acts by peristalsis to move the sperm along. Now scan over the section looking for tubules of the efferent ducts, which connects the rete testis to the epididymal duct. The efferent duct tubules are often (but not always) smaller than epididymal tubules, and their epithelium varies considerably in height, giving the tubule lumen a characteristic irregular or “star” shape. The epithelium is generally simple columnar, and consists of two cell types, taller cells have with cilia and shorter cells without cilia. The efferent duct is the only portion of the male tract displaying true, motile, cilia. These tubules may also have a thin layer of smooth muscle around them. Efferent ducts can be seen in slide #270 in a small region amongst the epididymis. III. SPERMATIC CORD284 spermatic cord H&E [DigitalScope] This is a cross section through a spermatic cord, such as you will see in the gross anatomy laboratory. On one side of the section you will see a cross section of the ductus (or vas) deferens [example], which has a circular lumen, lined by a pseudostratified epithelium and surrounded by a very thick wall of smooth muscle. Elsewhere you will see sections through two or more branches of the testicular artery, surrounded by connective tissue that contains numerous veins of the pampiniform plexus [example] (the veins are rather flattened and contain dark red blood). What is the function of the pampiniform plexus? The testicular artery has a typical internal elastic membrane and prominent circular smooth muscle coat (comprising the tunica media). The veins of the pampiniform plexus lack the internal elastic membrane, and their walls are somewhat less muscular. The blood in the vessels may have black particles in it, an artifact of the fixation procedure. The association of the veins of the pampiniform plexus with the testicular artery constitutes a countercurrent exchange system to cool the blood somewhat on its way to the testis. In the connective tissue you will find nerves and, around the periphery of the section, some cross-sectioned bundles of smooth (dartos) [example] and skeletal (cremaster) muscle [example]. IV. SEMINAL VESICLE075 seminal vesicle H&E [DigitalScope] These are cross sections through a seminal vesicle, which you may remember from gross anatomy is a rather sacculated and contorted tube (slide 75 is also the slide we used to study parasympathetic ganglia, which are readily observable in the wall of this organ). Study the section with your light microscope, noting the moderately-abundant smooth muscle in the wall. The epithelium of this gland lies on the surface of interconnecting mucosal folds that extend into the lumen from the muscular wall. The sparse connective tissue within the folds constitutes the lamina propria of this mucosa. The epithelium, which may be either simple columnar or pseudostratified columnar, produces a secretion (including fructose, ascorbic acid and other components) which is expelled from the gland by contraction of the muscular wall during ejaculation, constituting about 50-80% of the semen. V. PROSTATE GLANDUMich 281-1ex prostate Masson [DigitalScope] The prostate in an adult is about the size and shape of a chestnut and contains 15-30 tubuloalveolar glands that empty separately into the prostatic urethra. The most important structures to see on the slide are the prostatic glands that are present over most of the section. The glands are embedded in a connective tissue that includes abundant smooth muscle, best appreciated in the trichome-stained section (recall that collagen fibers will stain blue-green whereas smooth muscle is pink with deep red nuclei), which produces the pulsations of the prostate that expel the content of the glands during ejaculation. The epithelium of the glands is simple columnar (there may be a few basal cells), and the cells differ greatly in height to give the epithelium a folded appearance. The epithelial cells secrete various components of the semen (including citric acid and acid phosphatase).
|
||